In Bardarash camp, Premiere Urgence Internationale improved the quality of mental health services
Since December 2019, Première Urgence Internationale managed for nine months the provision of primary free health care services in the reopened camp of Bardarash, Kurdistan region of Iraq. The teams ensured individual mental health follow-up and counselling, as well as training of Iraqi doctors to improve the services provided inside the camp.
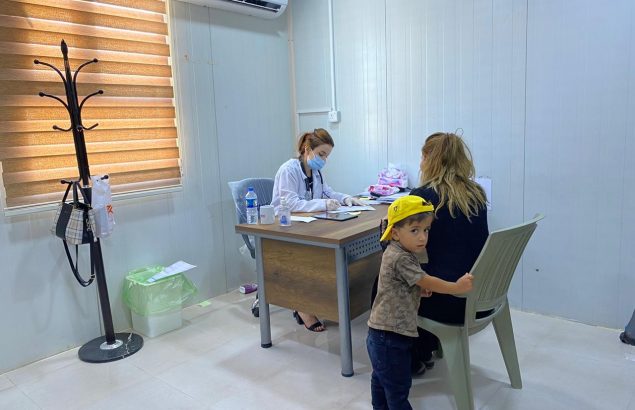
© Première Urgence Internationale | July 2020
In October 2019, the Turkish military operation in North East Syria led to mass displacement of the population to the South and the West of Syria, as well as towards the East and into Iraq. The Kurdistan regional government reactivated its contingency plan for the influx of Syrian refugees, and the humanitarian community established reception centres at the aforementioned border points. After accommodating the first few families in Domiz camp (Dohuk governorate) as a temporary measure, the authorities announced that Bardarash camp would reopen to face the high influx of refugees.
Première Urgence Internationale was the first actor to be present in Bardarash camp in 2014, providing integrated health; water, sanitation and hygiene; as well as psychosocial support until its closure in 2017. After a handover with Médecins sans Frontières, Première Urgence Internationale took over Bardarash camp’s primary health care center from 1st of December 2019.
As of April 30th 2020, 21,540 individuals had arrived to the Kurdistan region of Iraq. The on-going COVID-19 pandemic put even more strain on the health authorities, which are even more dependent and in demand for NGOs to continue supporting the vulnerable in-camp populations.
Recruitment and training of medical specialists
To address the mental health needs of the Bardarash camp population, and despite some challenges related to the availability of psychiatrists, Première Urgence Internationale was able to recruit one part-time psychiatrist, working in close collaboration with the NGO’s mental health teams and especially the deputy coordinator. Throughout the project, Première Urgence Internationale also provided training to a general practitioner doctor, Dr Sara, who was trained on the standard mental health gap.
Première Urgence Internationale’s Deputy Coordinator ensured a close supervision of the trained doctor, including weeks of clinical supervision and on-job training. Following which, Dr Sara is now able to assess, identify and manage patients with mental health issues, as well as prescribing some psychotropic medication, in addition to the general provision of support to physically ill patients. The remaining patients continued to be followed by the external psychiatrist and/or by the NGO teams.
“After 3 months of regular and intensive supervision by Première Urgence Internationale’s Deputy coordinator, Dr Naseem, I’m now able to treat most of mental health cases. Currently, we have more than 40 opened cases managed by me and six complicated cases that need psychiatric consultation managed by Dr. Naseem. Each case is discussed and followed during a weekly meeting.”
Dr Sara, general practitioner trained to mental health in Bardarash camp.
Referrals to specialized structures when needed
For patients in need of more intensive counselling, further laboratory investigation or hospital admission, Première Urgence Internationale developed a reliable referral pathway to enable these patients to be referred from the camp’s primary healthcare center to the mental health regional center. Therefore, two psychiatrists identified as focal points for referrals are receiving patients from Première Urgence Internationale’s facilities on a weekly basis, through free of charge transportation service.
Première Urgence being the main mental health actor in the camp, other partners are referring patients in need of mental health assessment and/or psychotropic treatment to Première Urgence Internationale’s teams. The NGO is conducting referrals to other actors for these patients in need. In terms of psychosocial support and counselling services, patients are mainly referred to the SEED Foundation for one-to-one and family support sessions, peer-to-peer support, and group interventions. Première Urgence Internationale and the SEED Foundation maintain close collaboration with regular technical meetings for referral purposes, briefing each other with the latest update and addressing any emerging challenges.
“Most of our mental health patients are improving”
According to Dr Lava, Manager of the camp’s primary health care center, “Most of our mental health patients are responding and improving nicely and they are highly strict to our management plan. I am also observing the improvement in the quality of service provided and how the service became more accessible and less stigmatized to the surrounding communities across the camp”.
As of July 2020, Première Urgence Internationale is now managing more than 50 patients in a comprehensive way, providing psychoeducation, psychiatric counselling and psychotropic medication when needed.
Due to the psychological impact of COVID-19, and given the particular vulnerability of the camp population, more incidents related to suicidal ideation, including attempts, have been reported in general. Thanks to the comprehensive treatment approach and a close follow-up by Première Urgence Internationale’s mental health staff, no fatality was reported among the registered patients.
Despite access challenges due to lockdowns and access restrictions imposed to contain the virus, Première Urgence Internationale mental health staff always maintained contact with beneficiaries, sometimes ensuring a follow-up via phone.
These activities were implemented by Première Urgence Internationale thanks to financial support from the French Government, through the CDCS (Crisis and Support Centre – French Ministry for Europe and Foreign Affairs). From end of August, 2020, Première Urgence Internationale will hand over the camp management to another local partner.