Rejoignez-nous
Première Urgence Internationale est toujours à la recherche de nouveaux talents pour étoffer son équipe, que ça soit au siège en France ou dans nos 25 pays d’intervention. N’attendez plus, rejoignez-nous !

Urgence Liban
La situation est dramatique.
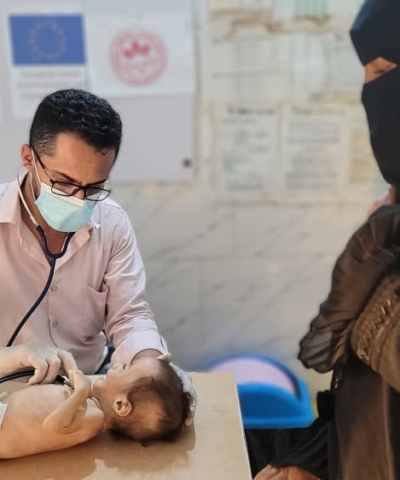
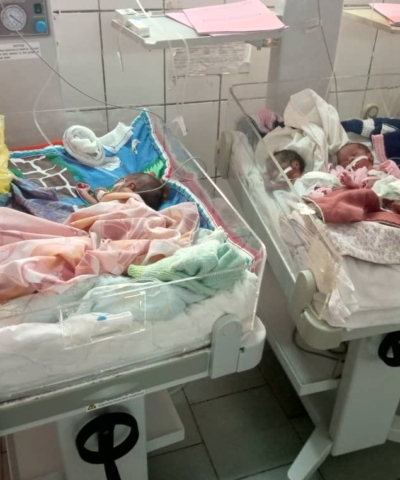
Dès les toutes premières heures de la crise, les équipes de Première Urgence Internationale se sont mobilisées sans relâche. Présentes à Baalbek, Hermel, Beyrouth ou encore dans le sud du pays, près de la frontière israélienne, violemment touchée, elles agissent avec un engagement exceptionnel pour venir en aide aux civils pris au piège des violences.
Votre don à notre Fonds d'Urgence nous permet de donner les moyens à nos équipes d’intervenir rapidement et efficacement.
Travailler chez Première Urgence Internationale, c’est…
- S’engager au sein d’une association humanitaire forte de 40 années d’expertises dans la réponse d’urgence et de post-urgence auprès de populations civiles en situation de crise dues à des conflits armés, des aléas climatiques ou des situations d’effondrement économique.
- Adopter une approche bienveillante et centrée sur les besoins des communautés locales et favoriser un environnement de travail respectueux et humain.
- Etre proche du terrain où chaque jour apporte de nouveaux défis et opportunités.
- Travailler en équipe, avec des collègues impliqués qui collaborent étroitement pour atteindre des objectifs communs. Ensemble, nous nous engageons à apporter des solutions durables et à faire une différence tangible sur le terrain.
Première Urgence Internationale a obtenu le label « Happy Trainees » trois années consécutives, attestant de son engagement envers la qualité de l’accueil et du développement de ses employés ayant le statut de stagiaire ou d’alternant. Cette reconnaissance, basée sur les avis des personnes concernées souligne l’environnement de travail positif et enrichissant offert par Première Urgence Internationale.


Christelle André
Directrice des Ressources Humaines © Première Urgence Internationale
“La prise en compte de l’humain et le plaisir de travailler ensemble sont essentiels pour mener à bien nos missions.”
Première Urgence Internationale est une ONG à taille humaine, accessible tant au niveau du siège que des missions. Rejoindre Première Urgence Internationale, c’est s’engager dans une aventure collective.
Faire carrière
S’investir dans l’aide humanitaire ne signifie pas forcément travailler sur le terrain. Il existe de nombreux métiers qui s’exercent au siège et qui sont tout autant indispensables à la réalisation de nos projets sur le terrain.

Travailler au siège ou sur le terrain
Chez Première Urgence Internationale, nous n’envoyons jamais de bénévoles sur le terrain. Même avec une grande volonté, cela n’est pas suffisant : les postes sur le terrain nécessitent des compétences très précises et de nombreuses formations et cursus universitaires répondent à ces besoins.
Les postes de terrain ouverts aux expatriés internationaux sont généralement des postes de coordination, de gestion de projet et de management. Ils représentent actuellement environ 220 postes répartis dans nos 25 pays d’intervention.
Les équipes de nos 25 missions sur le terrain sont composées de salariés nationaux directement recrutés dans les pays d’intervention. Ils représentent environ 3 000 postes à travers le monde.
Mais travailler dans l’humanitaire, ça n’est pas que travailler sur le terrain. Pour mener à bien nos projets, nous avons besoin de talents au siège sur des fonctions support : Communication, Systèmes d’Information, Ressources Humaines, Finances, Logistique, Services Généraux. Si ces postes ne s’opérèrent pas forcément sur le terrain, ils restent en lien étroit avec nos collaborateurs à travers le monde. Actuellement, 140 personnes travaillent au siège de Première Urgence Internationale juste à côté de Paris, à Asnières-Sur-Seine.
Favoriser l’évolution et la mobilité
Première Urgence Internationale accompagne le parcours professionnel de ses collaborateurs en offrant de nombreuses opportunités d’évolution interne, de croissance et de développement continu et en favorisant la mobilité terrain/siège.
La formation est une priorité pour nous car elle est essentielle pour améliorer les compétences, l’efficacité et la motivation de notre personnel. En investissant dans le développement professionnel de nos équipes, nous garantissons une meilleure qualité d’intervention et une plus grande adaptabilité aux défis humanitaires.
Si vous souhaitez avoir plus d’informations pour vous former et travailler dans l’humanitaire, vous pouvez vous rendre sur le portail de notre partenaire solidaire-info.org
Rejoignez-nous
Notre politique RH
Première Urgence Internationale offre de nombreux avantages à ses collaborateurs et a bâti sa politique RH sur 5 piliers :
- Equité et non-discrimination
- Transparence
- Objectivité
- Adaptabilité
- Confidentialité